Call us today: 1 (210) 615-8308

Colon Cancer Screening
Colon cancer affects 134,000 people per year in the United States and causes the death of 55,000 patients per year. This makes colon cancer the #2 cancer killer in the United States. Almost all colon cancers start out as a polyp on the inside wall (lumen) of the colon. Polyps start out as small wart-like bumps the size of an unground peppercorn.
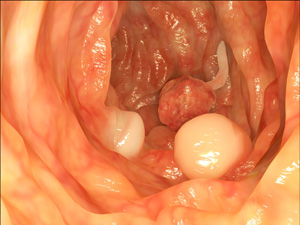
Colon Polyps
Over a period of 5-10 years, some of these polyps continue to grow up to 1-2 inches in diameter. At any time a microscopic size cancer (adenocarcinoma) may develop somewhere on the polyp. This usually will occur in polyps greater than 1 cm (a little less than 1/2 in.) in diameter. Once a cancer starts, it will eventually spread throughout the polyp, into the wall of the colon, then through the wall into surrounding tissues, lymph nodes, and possibly to the liver and/or lungs.
We don’t know what percent of polyps become cancers. Approximately 40% of people over the age of 50 have polyps and about 5% of the population will eventually develop colon cancer so we guess that 10 – 15% of patients with polyps will eventually develop colon cancer.
We also don’t know the factors involved in what causes polyps or what causes polyps to be malignant (cancerous). Much of the risk is genetic. This is some weak evidence that you are more likely to develop colon cancer if you are overweight, smoke, drink excessively, don’t exercise, and eat a diet that is high in animal fats and low in fiber, fresh fruits, and vegetables. Some supplements that have been proposed to lower the risk of colon cancer (but none proven) include calcium (1200 mg/d), fiber supplements, vitamin E (200-400 IU/d). vitamin C (500 – 1000 mg/d), folic acid (400 mgm/d) and NSAID/aspirin use.
The best way to detect colon cancer is to undergo periodic screening on order to detect polyps before they become malignant. Whenever a polyp is detected, the patient should have a complete colonoscopy to look for any other polyps and remove all of them. Taking into consideration risk and cost, the best way to do this (given our current knowledge and understanding which will certainly change in the future with new studies and technology) is to undergo a complete colonoscopy at age 50 and every 10 years after that until age 80. Some patients are at higher risk due to family history of colon cancer or polyps and need more frequent exams beginning at age 40 or earlier. Please let us know if you have colon cancer or polyps in the family. Once polyps are detected, you should have a colonoscopy every 3-5 years to detect new polyps.
If your insurance does not pay for screening colonoscopies and you do not have an acceptable reason (to the insurance company) for colonoscopy (such as rectal bleeding, diarrhea, a change in bowel movement, etc.) then the next best choice is to either pay out of pocket or undergo a barium enema/ flexible sigmoidoscopy every 5 years.
Even if all screening recommendations are followed, no one can guarantee a patient will be cancer free. Some polyps are merely impossible to find due to location or associated technical difficulties such as the colon not being completely clean before the exam, sharp turns, diverticular disease, or colonic spasms. Rarely, a cancer will develop from a flat lesion (not a true polyp) of the colon, which is very difficult to detect.
Eating a healthy diet, exercising, not smoking, limiting alcohol consumption to no more than 2 drinks per day, and avoiding obesity is a good way to prevent heart disease, strokes, and many cancers. However, the most effective method of preventing colon cancer is regular screening. Please consider undergoing these tests, not only for yourself, but your loved ones as well.